
Footcare Conditions
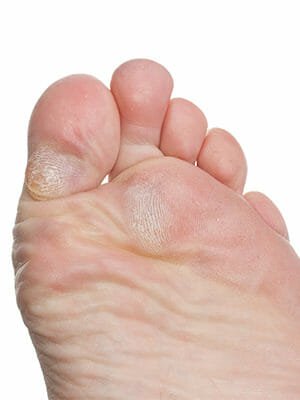
What is hard / thick skin in the bottom of my foot?
What
Callus and corns are thickened and hard skin that is formed in areas of excessive pressure. A callus refers to diffuse area of thick skin while a corn is thicker and localized to one area. In general, calluses are not harmful, but can be painful and may occasionally lead to an infection or ulceration of the skin if not treated.
Why
Calluses or corns can be due to:
- ill-fitting shoes / socks
- not wearing socks
- sweaty feet
- barefoot walking
- individuals with foot problems (i.e. Bunions, clawed toes, hammer toes and or arthritic foot with less padding).
Treatment
Never cut corns or calluses with any instrument, and never apply home remedies. Seek medical advice from your Chiropodist in managing the right treatment option appropriate for you.
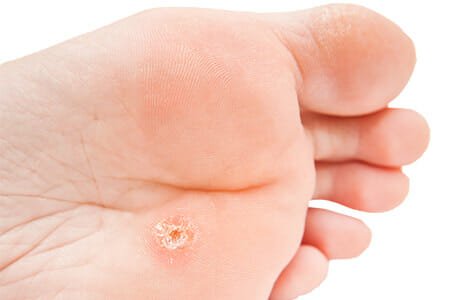
What is a lesion in the bottom of my foot with black dots?
What
Warts are noncancerous skin growths caused by a viral infection known as HPV (Human Papillomavirus) and in the foot they usually occur on sole (plantar) of the foot. They can also fuse or develop into clusters called mosaic warts. They usually resemble a cauliflower with tiny black dots that can bleed at times.
Why
The virus attacks compromised skin through direct contact, entering through tiny cuts, abrasions in the skin. After the infection, the virus can become visible within weeks or take months. Warts can be transmitted by touching, scratching of one part of the skin to another, friction that removes a portion of the organism to another surface or organism or through blood. Usually these viruses are found in damp areas: swimming pools, hot water tubs, public shower floors and benches or locker rooms.
Treatment
Warts can be very resistant to treatment and have the tendency to reoccur. Over the counter treatments can be dangerous as they are not strong enough to destroy the wart, but harsh enough to destroy surrounding healthy tissue. Please contact our office to help effectively treat your warts.
Preventing
- Avoid direct contact with warts, both form other persons or other parts of the body
- Avoid barefeet except on sandy beaches
- Change socks and footwear daily
- Check your children’s feet daily
- Keep your feet dry and clean

Why does my heel on my foot hurt?
What
Although there are many different causes for heel pain, Plantar Fasciitis is the most common cause of heel pain. Plantar Fasciitis is an inflammation of the band of connective tissue (the plantar fascia) that extends from the heel to the toes. It is sometimes referred as the “heel spur syndrome” – when a bone spur is presented on the heel – presented on an X-ray. And the symptoms can be a combination of:
- Pain in the bottom of foot
- Pain at the first step of prolonged rest (i.e. from sleep or sitting)
- Pain in the arch of the foot
Why
There are many causes to plantar fasciitis which can range from:
- High to low arches
- Poor footwear
- Weight gain
- Sports injuries
- Over-use injuries
- Poor biomechanics
Treatment
Since it is associated with inflammation, it is best to follow
- R- rest
- I – ice
- C- compression
- E- elevation
If symptoms do not resolve, contact our clinic for a thorough physical examination for accurate diagnosis, as there a few conditions that have similar presentation as plantar fasciitis. Furthermore, we can discuss other treatment modalities and options that may work better for you.
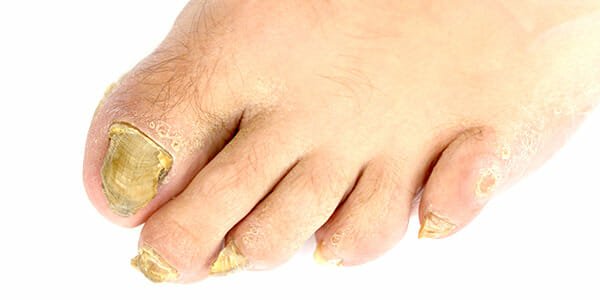
Why toenails becoming thick and discoloured?
What
Thick and discoloured toenails are often caused by a fungus that invades the nail. Is the most common nail condition, in which the nail begins to discolour itself. It can start as white or yellow discolourtion and if left untreated, it can spread to other nails or cause the infected nail to become thick, crumbly and or cause separation of the nail from the nail bed. You may also feel pain in the toenail and detect a slightly foul odour.
Why
Dermatophyte fungus is the main cause to nail fungus, however yeast and molds can also contribute to the problem. Fungus thrives on dark, moist environments and can invade your skin through small cuts or a small separation between the nail and nail bed. In severe cases it can be painful and can cause permanent damage to the nail. Some of the risk factors include:
- Elderly with compromised circulation
- Excessive sweating in the feet
- Working in humid or moist environment
- Poor feet and footwear hygiene
- Walking barefoot in damp communal areas
- Trauma to the nail
- Surrounding Skin condition, infection
- Sharing nail clippers, footwear, socks with someone who is infected with nail/skin fungus
Treatment
Treatment for fungal toenails ranges from topical, laser to oral medications. However, nail fungus can mimic many other dermatological conditions. Sometimes thick nails are not fungus at all but are due to trauma either from something dropping onto the toenail or shoes that are too tight, especially athletic shoes. Athletic shoes should be fit so that there is a full finger’s width in front of the longest toe while standing.To better diagnose and discuss different treatment options best suited and tailored to your health, please contact our clinic.

What are bunions?
What
Bunions, also known as Hallux Abductovalgus is a bone deformity caused by an enlargement of the joint at the base and side of the big toe. Bunions form when the toe moves out of place. The enlargement and the protuberance cause friction and pressure against footwear leading to irritation or inflammation. If left untreated, the bunion can further enlarge and overlap adjacent toes, develop bursitis, cause hammer toes, and or lead to arthritis in the joint, making overall walking uncomfortable.
Why
Bunions are not hereditary, but can run in families due to faulty foot structure and mechanics. Other reasons as to why they form can be: ill-fitted footwear – usually too narrow, foot injuries and neuromuscular problems.
Treatment
Since bunions are bony deformities, they do not go away on their own, the best is to address the underlying cause. Depending on the severity of the bunions, treatment options can range from therapeutic and mobilization modalities to help with pain and function, orthotics which will help stop the progression of the bunion and help with pain and last surgery. Surgery is the only permanent solution for bunions, however, orthotics are used after surgery as well to help prevent the reoccurrence of the bunion. For more information on appropriate treatment for you, contact our clinic for an appointment.
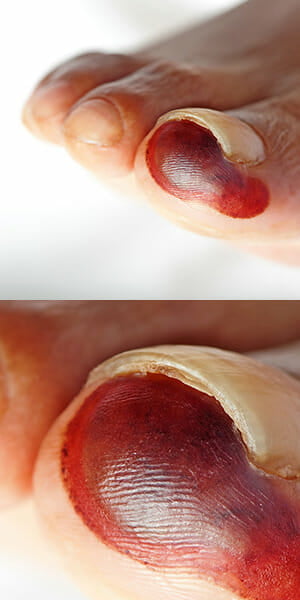
My toe nail is red and swollen, is this infected?
What
Ingrown toe nails is a common condition affecting mainly the big toenails, which occurs when the corner or side of a toenail grows into the skin, causing pain, redness, swelling and often an infection.
Why?
Ingrown toenails can result for many reasons, some include:
- Cutting toenails too short or not straight across
- Leaving a spike in the nail
- Wearing improper footwear
- Trauma to the nail
- Fungal / thickened toenails
- Having unusually curved nails – inherited /hereditary condition
- Poor foot hygiene
- Abnormal gait
- Foot or toe deformities (bunions, hammer toes)
- Congenital toe deformity
- Obesity
- Pregnancy
- Excessive sweating or swelling of the feet
Treatment and prevention
Conservative treatment include Epsom salt soaks, elevation, and proper foot hygiene. However, sometimes based on the length and severity, antibiotics or minor surgery maybe necessary. If home treatments are not successful within a week, seeking podiatric medical advice is recommended to further assess the cause of the ingrown and discuss the best treatment route.
Note: Persons with diabetes or compromised immune system should immediately consult a chiropodist / podiatrist / physician before any self conservative treatment.

How does diabetes affect my feet?
What
Diabetes is continued high levels of blood sugar which over- time can cause permanent damage to everything from blood vessels (diabetic angiopathy), nerves (diabetic neuropathy) and even sweat glands of the skin (autonomic neuropathy). Uncontrolled diabetes greatly reduces one’s ability to fight off infections and slows any healing down.
Why?
Diabetic feet are considered high risk feet – meaning diabetic individuals are at high risk of developing foot problems and diabetic infections in the legs and feet. Some factors are:
- Poorly fitted footwear
- Red spots
- Sore spots, blisters
- Corns, calluses
- Thick and ingrown nails
- Flat feet, bunions, hammer toes, clawed toes
With such risk factors and ones inability to heal efficiently and sense minor injuries – it can lead to serious problems such as losing a toe, foot, or even a leg.
Treatment
At FCO we provide a thorough examination at least once year to identify high risk diabetic foot conditions. We provide routine foot care needs for diabetic patients to help prevent diabetic foot complications. We also help manage wounds if they develop and we work with your physician if necessary to achieve best optimal care. Foot health plays an important role in the well being of a diabetic. Although diabetes affects the entire body, the lower extremity is often affected first.
To maintain proper diabetic foot care it is important to:
- Wash your feet daily using lukewarm water and mild soap
- PAT dry
- Dry carefully between and underneath your toes
- Apply an emollient daily, avoiding between toes
- If your feet are moist and sweaty – use a foot powder, especially between toes
- Change socks / stockings daily
- Examine your feet carefully everyday for bruises, cracks, redness, swelling and if you are not able to reach, get someone else to help
What could cause a toe with sharp and numbness symptoms?
What
Morton’s neuroma is a painful condition that affects the ball of the foot. This is an irritation and inflammation of the nerve, usually between the 3rd and 4th toes. With this condition one may feel as if they are standing on a pebble or on a fold in their sock. At times, it can be also described as a sharp, burning pain or numbness in the ball of the foot travelling to the toes.
Why
Factors that play a role in one developing a neuroma are:
- High-heeled shoes have been linked to the development of Morton’s neuroma, which is why it is most common amongst women.
- Tight footwear,especially in the toe-box.
- People with certain foot deformities – bunions, hammertoes, flatfeet, or more flexible feet.
- Activities that involve repetitive irritation to the ball of the foot.
Treatment
Conservative treatment involves footwear modification and custom made orthotics. If the symptoms still continue, steroid injections and oral anti-inflammatory medications can calm the nerve irritation. Last resort is surgical excision. If you are concerned with the tingling, burning, sharp pain or numbness when you walk, contact FCO. We’ll perform a careful examination and present your options for best treatment tailored to your health.

What is a Custom Orthotic?
What
A custom orthotic is a shell or support made out of various materials which, when placed within the shoe, supports the foot and maintains normal foot function. Custom orthotics should not be confused with prefabricated “arch supports”. A custom orthotic is made specifically for your foot. When you are seen by our clinic, the Chiropodist may suggest a custom orthotic based upon your specific problem. This includes a biomechanical evaluation and a non weightbearing 3D scan or a plaster cast mold of your feet. Based on your evaluation, the Chiropodist will write a prescription detailing the choice of materials (rigid or flexible), the proper biomechanical alignment or tilt of the orthotic and modifications which take into consideration your complaint, occupation, sport, and preferred shoe.
Why
Feet are an amazing complex structure consisting of one quarter of the body’s bones (52 bones in both feet) held together with ligaments, muscles, tendons, and fascia helping you efficiently through thousands of steps. The average person takes more than 3000 – 10,000 steps in a single day. However, sometimes improper foot alignment, skeletal imbalances, medical conditions, inappropriate footwear can cause pain throughout your body by over stressing muscles, tendons, bones and joints, leading to an inefficient gait. To address such biomechanical defaults, at times custom made orthotics are prescribed to alter the way your feet interact with the ground (gait). They work to control your foot motion and weight distribution.
Treatment
If you have a concern with your current custom orthotic – or feel you may have a need for one – let FCO know to ensure you get the best fitting orthotic possible. Contact us today.


